ORIGINAL ARTICLES
Aim. To study the significance of monitoring high-sensitivity troponin I (hs-cTnI) for predicting anthracycline-induced left ventricular (LV) dysfunction in the treatment of breast cancer in patients with moderate and low risk of cardiotoxicity (CT).
Material and methods. The study involved 49 patients with breast cancer aged 50±10 years who underwent neoadjuvant or adjuvant chemotherapy, which included doxorubicin at a course dose of 60 mg/m2 and an average cumulative dose of 251±60 mg/m2. The level of hs-cTnI was determined by an ultrasensitive method before the start of chemotherapy, after each course of anthracyclines and in 18 patients before the administration of anthracyclines. The level of hscTnI >0,017 ng/ml was considered elevated. Echocardiography was performed before the start of chemotherapy, after the end of anthracycline therapy, and every 3 months for 12 months thereafter. CT was defined as a decrease in LV ejection fraction (EF) by ≥10% to <53%.
Results. CT risk before chemotherapy was considered low and moderate in 96% of patients. An increase in hs-сTnI was detected ≥1 times in 56,8% of patients: before chemotherapy — in 13,5%, after 1 and 2 courses of anthracycline therapy — in 13,9%, after 3, 4, 5 and 6 courses — in 44%, 62%, 71% and 66% of patients, respectively. The levels of hs-cTnI before and after administration of anthracyclines did not differ significantly. The development of LV dysfunction was observed in 16,3% of patients. There were following prognostic significance of an increase in hs-cTnI at any time of chemotherapy for a decrease in LV EF: sensitivity — 87,5%, specificity — 50%, the positive predictive value — 28%, the negative predictive value — 94,7%. The closest relationship was noted between CT and hs-cTnI value before the start of chemotherapy (β=0,45, p=0,005) and after the 3rd course of anthracycline therapy (β=0,56, p=0,002).
Conclusion. An increase in hs-cTnI level before and during anthracycline thera py in patients with a low risk of cardiotoxicity has a prognostic value in relation to the development of left ventricular dysfunction. Hs-cTnI assessment should be performed before the start of therapy, and then starting from the 3rd course of anthracycline therapy in all patients, regardless of the risk of cardiotoxicity.
Aim. To determine a possible prognostic marker for adverse cardiovascular events in patients with gastric cancer by studying the early and long-term effects of multiagent chemotherapy (MAC) on the structural and functional vascular wall parameters.
Material and methods. The study included 25 patients with newly diagnosed gastric cancer who received courses of chemotherapy with platinum-based agents and fluoropyrimidines. All patients before, immediately after MAC courses and in the long-term period underwent a non-invasive assessment of vascular wall and endothelial function (photoplethysmography (PPG)). In the survivors’ cohort, a correlation analysis was performed to assess the risk of future cardiovascular events depending on changes of PPG parameters.
Results. Before the MAC courses, cancer patients had endothelial dysfunction (mean occlusion index, 1,7 (1,4; 1,9), N>1,8) and structural vascular wall disorders (mean stiffness index, 8,9 m/s (7,7; 9,7), N<8 m/s, mean reflection index, 32,4% (27,5; 37,7), N<30%). All indicators significantly worsened after MAC in the form of endothelial dysfunction progression and vascular remodeling: mean occlusion index, 1,3 (1,2; 1,5) (p<0,0002), stiffness index, 10,3 m/s (9,5; 11,2) (p<0,0001), reflection index, 40,2% (35,5; 43,6) (p<0,001). Long-term follow-up averaged 2,9 years (2,3-3,7 years). All-cause and cardiovascular mortality was 32% and 12%, respectively. Nine patients developed a cardiovascular events (CVEs) (de novo, progression of prior CVD). Significant changes of vascular indicators in the long-term period was not revealed. A trend towards association between increased reflection index and a higher probability of cardiovascular pathology was revealed (OR 1,20, 95% CI 1,01-1,55, p=0,081).
Conclusion. In this study, for the first time, a comprehensive assessment of the effect of MAC on endothelial dysfunction and vascular stiffness, including, in the long-term follow-up period, was carried out in patients with gastric cancer. A significant aggravation of all parameters of vascular remodeling immediately after treatment in the absence of their significant dynamics in the future has been proven. A possible prognostic marker, namely the reflection index, of an unfavorable cardiac outcome in patients with gastric cancer has been identified, which requires further study.
Aim. To evaluate the early manifestation of cardiotoxicity after the first course of multiagent chemotherapy (MAC) using echocardiography with an assessment of the left ventricular ejection fraction (LVEF) and global longitudinal strain (GLS).
Material and methods. The study included 49 cancer patients with elective MAC.
Results. After the first administration of a therapeutic dose of chemotherapy, a decrease in LVEF ≥10 and GLS >15 was demonstrated in more than 6,1% of patients, as well as a subclinical decrease in LVEF ≥5% in 22,4% and a decrease in GLS ≥12% in 24,5%.
Conclusion. In cancer patients, after the first course of chemotherapy, GLS dynamics should be assessed during echocardiography as a marker of myocardial dysfunction.
Aim. To evaluate the information value of a complex of clinical and biochemical parameters of myocardial damage in predicting the development of transmural myocardial damage according to magnetic resonance imaging (MRI) in patients with acute myocardial infarction (AMI).
Material and methods. The study included patients admitted to the emergency cardiology department with acute coronary syndrome. All patients underwent invasive coronary angiography, laboratory tests, and dynamic determination of cardiac biomarkers. In the interval of 6,1±4 days from admission to the hospital, patients underwent contrast-enhanced cardiac MRI. According to the pattern of delayed contrast enhancement, patients were divided into two groups: with a transmural and subendocardial pattern.
Results. The mean age of patients was 62,5±10,5 years, while 27 (71,1%) had ST-segment elevation AMI. Among the risk factors for coronary artery disease, dyslipidemia (89,5%), hypertension (68,4%), and smoking (57,9%) were the most common. Creatine phosphokinase-MB (CPK-MB), serum high-sensitivity cardiac troponin I (cTnI) and C-reactive protein (CRP) values after 24 h were significantly higher in patients with transmural hyperenhancement. Moderate positive relationship was found between the global size of left ventricular (LV) damage according to MRI data and the levels of CPK-MB after 24 h and 4 days, as well as with CRP after 24 h, 4 and 7 days, and cTnI level after 24 h and 4 days. In the group of patients with transmural pattern, the global size of LV damage was significantly higher. Patients of this group were characterized by higher prevalence of microvascular obstruction. In a univariate regression analysis, there were following significant predictors of transmural myocardial damage: CPK-MB after 4 days (p=0,023) and ST segment elevation (p=0,029). Multivariate regression analysis showed that the only independent predictor of transmural myocardial damage was an increase in CPKMB after 4 days (p=0,023).
Conclusion. An independent predictor of LV transmural damage in AMI was an elevated level of CPK-MB after 4 days. However, this laboratory marker had unsatisfactory information completeness and predictive quality. In this regard, cardiac MRI in patients with AMI, compared with the standard clinical assessment, can be considered preferable for assessing the depth of myocardial damage, risk stratification, and prognosis.
Aim. To analyze the results of thrombectomy in lower-extremity ischemia in patients with coronavirus disease 2019 (COVID-19) and respiratory failure of different severity.
Material and methods. This retrospective, cohort, comparative study for the period from May 1, 2020 to March 1, 2022 included 305 patients with acute lower-extremity ischemia and COVID-19. Depending on the type of oxygen support, three groups of patients were formed: group 1 (n=168) — nasal oxygen insufflation; group 2 (n=92) — non-invasive ventilation (NIV); group 3 (n=45) — artificial ventilation (AV). Thrombectomy was carried out according to the standard technique using Fogarty catheters (3F-6F — depending on the vessel size). After the diagnosis was established before and after the start of surgical treatment, all patients received the following therapy: Unfractionated IV heparin infusion at an initial rate of 1000 U/r, adjusted to maintain the activated partial thromboplastin time at 2-3 times the normal value; 2. Oral acetylsalicylic acid 125 mg; 3. Analgesics.
Results. Myocardial infarction and ischemic stroke were not detected in the total sample. The highest number of deaths (group 1: 5,3%, n=9; group 2: 72,8%, n=67; group 3: 100%, n=45; p<0,0001), retrombosis (group 1 : 18,4%, n=31; group 2: 69,5%, n=64; group 3: 91,1%, n=41; p<0,0001) and limb amputations (group 1: 9,5%, n=16; group 2: 56,5%, n=52; group 3: 91,1%, n=41; p<0,0001) was recorded in group 3 patients.
Conclusion. In patients receiving mechanical ventilation, COVID-19 have more aggressive course, which is expressed in an increase in laboratory para- meters (C-reactive protein, ferritin, interleukin-6, D-dimer), the severity of pneumonia and location of thrombosis in the tibial arteries. Among patients with COVID-19 receiving mechanical ventilation, the greatest number of rethromboses (91,1%), limb amputations (91,1%), and deaths (100%) are noted, which suggests the expediency of abandoning open thrombectomy in favor of anticoagulant/antiplatelet therapy in this cohort of patients. The development of arterial thrombosis in patients with COVID-19 receiving mechanical ventilation is an indicator of a high risk of death. Open thrombectomy in combination with anticoagulant/antiplatelet therapy is most effective in patients on nasal oxygen insufflation or NIV.
Aim. To study the traditional risk factors for cardiovascular disease (CVD), indicators of endothelial function and exercise tolerance in patients received complex treatment for cranial and craniospinal tumors in childhood, including radiation therapy.
Material and methods. We compared examination data of 48 patients who underwent treatment for brain tumors using cranial and craniospinal irradiation in childhood (mean age, 21,7±4,3 years, mean period after the end of treatment, 6,9±5,4 years), and 20 healthy volunteers. Examination methods included assessment of lipid profile, vascular stiffness and endothelial function using the Photoplethysmography and occlusion test, cardiopulmonary test, and in patients who underwent craniospinal irradiation, also echocardiography and duplex ultrasound of extracranial arteries.
Results. Compared to healthy individuals, patients after a brain tumor were found to have lower blood pressure, higher heart rate (HR), significantly lower exercise performance (peak oxygen consumption, 19,8±6,4 ml×min-1×kg vs 30,3±5,8 ml×min-1×kg, p<0,0001) and a higher prevalence of dyslipidemia (56% vs 5%, p<0,0001), as well as an increase in the augmentation index, indicating higher stiffness of large vessels (-7,3±16,3 vs -20,3±7,9, p=0,001), and a trend towards a decrease in the occlusion index (p=0,051). Echocardiography and duplex ultrasound revealed no radiation-associated abnormalities.
Conclusion. Determining the mechanisms and prognostic significance of the identified risk factors for CVD (dyslipidemia, decreased exercise tolerance, increased heart rate and vascular stiffness) in this category of patients requires further research. Regular monitoring of risk factors, primarily the lipid profile, and the use of preventive measures for individuals with an increased risk of CVD should be recommended.
GUIDELINES FOR THE PRACTITIONER
Aim. To study the effectiveness of exogenous phosphocreatine (EPCr) therapy in patients with heart failure (HF) with reduced and mildly reduce dejection fraction (EF).
Material and methods. The all-Russian prospective observational study BYHEART included 842 patients who underwent aEPCr therapy course. Before and after the course of EPCr therapy, the following studies were carried out: a questionnaire on the Minnesota Living with Heart Failure Questionnaire (MLHFQ) and the clinical assessment scale (CAS), transthoracic echocardiography with an assessment of the left ventricular EF, a 6-minute walk test, N-terminal pro-brain natriuretic peptide (NT-proBNP). All patients before the EPCr course received long-term optimal therapy for HF.
Results. Data analysis was carried out for patients in groups with heart failure with reduced ejection fraction (HFrEF) and with mildly reduced ejection fraction (HFmrEF) within the group depending on the course of EPCr treatment: subgroup A — patients who received EPCr therapy less than 20 g/course and subgroup B — patients who received EPCr therapy ≥20 g/course. The results obtained demonstrate an increase in the quality of life and exercise tolerance, an improvement according to the CAS, a decrease in NT-proBNP levels, and an improvement in left ventricular systolic function in patients with both HFrEF and HFmrEF during the course of intravenous EPCr therapy.
Conclusion. The use of EPCr is a promising tool in addition to optimal therapy in patients with HFrEF and HFmrEF.
The article presents epidemiological data on the high prevalence of hypertension and dyslipidemia comorbidity in the general population, as well as shows the leading role of these key cardiovascular risk factors in the development of cardiovascular events. At the same time, within the primary prevention, the adherence of patients to the lipid-lowering therapy remains low. Fixed-dose combinations (Lipertans) based on antihypertensive (amlodipine, perindopril) and lipid-lowering drugs (atorvastatin) can significantly increase the effectiveness of therapy.
EXPERT CONSENSUS
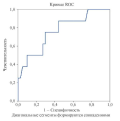
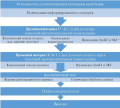
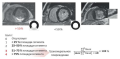
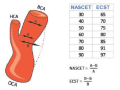
Carotid stenosis is a multidisciplinary problem that requires the involvement of a specialists’ team, including cardiovascular surgeons, neurosurgeons, endovascular surgeons, cardiologists, neurologists, and internists. In this consensus statement, a group of experts considered the main stages of diagnosing carotid stenosis, as well as discussed, the necessary prevention methods and features of choosing the optimal treatment approach. The aim was to provide concise and structured information on the management of patients with carotid stenosis. This document was developed based on the updated clinical guidelines of the European Society for Vascular Surgery and the American Association for Vascular Surgery, taking into account the consensus opinion of Russian experts.
CLINICAL CASE
Introduction. Cancer remains one of the most common causes of death in the world, second only to cardiovascular diseases. The use of novel chemotherapeutic and targeted agents has significantly improved the prognosis of this group of patients. However, this significantly increased the number of cardiotoxic complications of anticancer therapy, including arrhythmias, in particular atrial fibrillation (AF), which negatively affects the prognosis.
Brief description. The purpose of this article was to describe the case of a 64-yearold woman with central right lung lower lobe cancer. Upon admission to the chemotherapy department, the patient was first diagnosed with paroxysmal AF. After chemical cardioversion, the first course of multiagent chemotherapy (MAC) was performed as follows: paclitaxel 280 mg and carboplatin 450 mg, which was complicated by the development of recurrent AF episode. During subsequent MAC courses, arrhythmia episodes regularly occurred. During the next AF episode, the patient was hospitalized at the City Clinical Hospital № 51, where she died despite intensive therapy. Postmortem examination ruled out tumor invasion into the left atrium.
Discussion. For the AF development, the patient had prerequisites in the form of a significantly remodeled left atrial myocardium. Chemotherapy agents used as antitumor therapy are characterized by the common development of cardiotoxicity, including variety of arrhythmias. The occurrence of AF episodes coincided with the course of MAC, which suggested its cardiotoxic manifestations. Postmortem examination confirmed the high probability of an association between AF episodes and MAC.
Conclusion. The presented case illustrates the difficulties encountered by oncologists and cardiologists in determining the genesis and treatment of complex arrhythmias in cancer patients.
REVIEW
The spread of cardiovascular diseases has the nature of an epidemic, which is enhanced by lipid profile disorders, manifested by hypercholesterolemia. Numerous conventional pharmacological tools for lowering cholesterol associated with low density lipoproteins do not make it possible to achieve target values in various categories of patients. Inhibition of proprotein convertase subtilisin/ kexin type 9 (PCSK9) is a promising target in the management of patients with atherosclerotic diseases and includes two main tools — monoclonal antibodies (Alirocumab and Evolocumab) and a small interfering RNA drug (Inclisiran). The presented review is devoted to a comparative analysis of the efficacy and safety of drugs from these groups.
Chest pain is a typical manifestation of acute myocardial ischemia. The likelihood of death in myocardial infarction increases significantly as the pain to hospital times increase, Therefore, timely recognition of this symptom as a possible manifestation of ischemia, calling an ambulance and first aid before the arrival of ambulance team can play a vital role in saving lives. A review of modern principles and rules for first aid to patients with chest pain is presented, based on an analysis of international and national guidelines. We demonstrated the need and identified directions for improving the organization of first aid in this condition in Russia, as well as analyzed approaches to remote questioning and provision of instructions on first aid for chest pain by ambulance dispatchers by phone, Based on the comparative analysis of dispatcher guidelines and protocols and international guidelines on first aid for chest pain, a universal Russian-language dispatcher algorithm for remote care for chest pain has been developed, which is proposed for discussion and further testing as a potential component of a unified domestic dispatcher support program for first aid.
Cardiovascular and cancer diseases are an urgent problem in medicine due to their high prevalence and adult mortality throughout the world. The review article discusses important aspects of the comorbidity of cardiovascular and cancer diseases. In particular, epidemiological aspects and general risk factors are analyzed. Modern view on the main issues of primary and secondary prevention of the combination of these diseases is presented.
ISSN 2618-7620 (Online)